A common presentation in sports medicine and musculoskeletal practice is localized low back pain following barbell deadlifting, particularly during periods of rapid training progression such as the beginning of the new year. Patients often report acute or sub-acute onset during or shortly after lifting, with stiffness and pain localized to the lumbar region. In the absence of radicular symptoms, neurological deficits, or red flags, this presentation most often reflects mechanical low back pain involving the lumbar erector musculature and posterior ligamentous structures, including the supraspinous, interspinous, and iliolumbar ligaments (1,2).
Understanding the biomechanics and physiology behind this injury pattern allows clinicians to intervene in a way that restores load tolerance and movement confidence rather than reinforcing fear-based protection.
During barbell deadlifting, the lumbar spine is exposed to substantial compressive and shear forces that evolve with repetition, fatigue, and technique drift. Biomechanical analyses of repetitive deadlifting demonstrate that as volume and intensity increase, lumbopelvic coordination and trunk stiffness regulation become less precise, resulting in altered spinal loading patterns (3). Importantly, injury in these cases is rarely the result of a single catastrophic event; rather, it reflects the interaction of high mechanical demand, fatigue, and subtle changes in neuromuscular control (3,4).
Lumbar erector spinae strain typically occurs through fatigue-related overload. During the deadlift, the erectors function largely isometrically to resist spinal flexion and maintain trunk stiffness while the hips generate movement. As fatigue accumulates, extensor force production capacity and timing degrade. Even small increases in trunk flexion moment, such as bar drift away from the body or delayed bracing, significantly increase demand on the lumbar extensors, predisposing the tissue to microtrauma and protective tone (3,5).
Posterior ligamentous strain or irritation frequently co-exists with muscular strain. Posterior spinal ligaments serve as passive stabilizers and secondary restraints, not primary load-bearing tissues. When muscular stiffness momentarily drops under fatigue, load shifts toward these passive structures. Experimental and biomechanical studies demonstrate that repetitive or sustained flexion under load produces viscoelastic creep in posterior spinal tissues, temporarily reducing stiffness and increasing susceptibility to strain (6,7). This mechanism helps explain why symptoms often emerge later in a training session or following activity rather than during the first exposure.
In the first 24 to 48 hours following injury, symptom severity is often driven more by nociception and neural protection than by structural compromise. Local tissue irritation activates nociceptors and inflammatory mediators, while the nervous system responds by increasing trunk co-contraction to limit motion at the sensitized region (2,8). This protective stiffness is adaptive in the short term but may delay recovery if it persists and limits graded re-exposure to movement.
Clinically, these patients often present with sharp or focal low back pain, discomfort during transitions such as sit-to-stand or rolling, pain at end-range flexion or extension, and a subjective sense of instability without true weakness. Recognizing this presentation as mechanical rather than discogenic or neurological is critical, as it supports an active, load-management-based approach rather than prolonged rest (1,2).
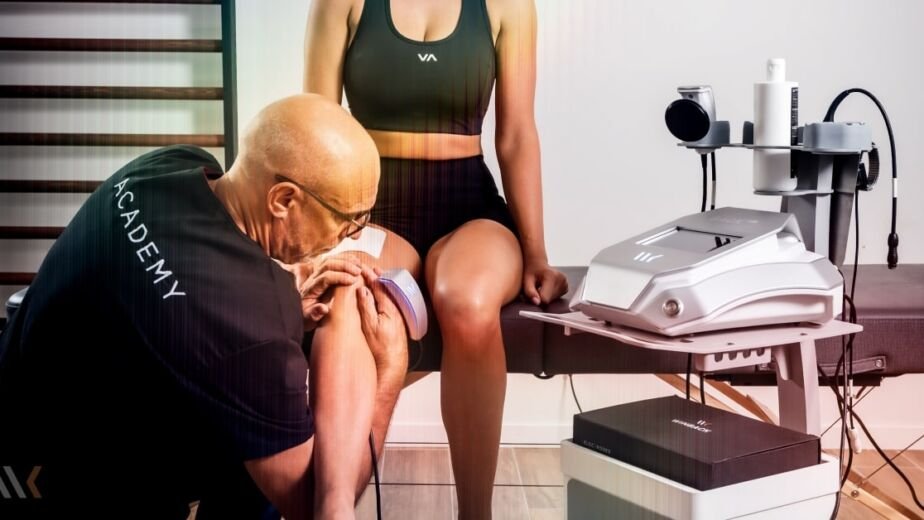
Early intervention should focus on reducing pain sensitivity, restoring tissue tolerance, and re-establishing efficient load sharing through the trunk. This framework aligns well with the physiologic effects of TECAR therapy when used as an adjunct to movement retraining.
Capacitive and resistive electric transfer therapy has demonstrated benefits in reducing pain and muscle stiffness in chronic nonspecific low back pain populations, including in double-blind randomized clinical trials (9,10). While these studies primarily examine chronic presentations, the physiologic mechanisms targeted—neuromodulation, improved circulation, and enhanced tissue tolerance—are directly relevant to acute and sub-acute mechanical low back pain. Clinical trials combining TECAR with manual therapy further demonstrate short-term improvements in pain and disability, supporting its role in improving movement readiness (11).
From a clinical standpoint, TECAR can be applied strategically to modulate tissue sensitivity and facilitate movement. Capacitive mode is typically used first to address superficial and intermediate tissues with higher water content, such as the paraspinal musculature and fascia. This reduces guarding and perceived threat, allowing the nervous system to tolerate motion. Resistive mode can then be layered to influence deeper posterior tissues and focal sensitized regions associated with ligamentous irritation, improving tolerance to load and shear.
Hi-TENS may be incorporated to further modulate pain and reduce neural drive associated with protective stiffness. The goal is not passive analgesia but rather enabling movement without triggering excessive guarding. EMS can then be introduced as a motor primer, commonly targeting the abdominal wall to improve anterior and lateral trunk contribution. In this context, EMS is not used to inhibit the erector spinae, but to redistribute load and improve neuromuscular timing so posterior tissues no longer carry disproportionate demand.
The versatility of Winback TECAR and addition of Care+ Programs create a therapeutic window in which patients can immediately engage in graded hinge exposure and trunk endurance work. This approach supports recovery by restoring efficient load sharing and movement confidence rather than reinforcing rigid bracing or fear avoidance.
In deadlift-related mechanical low back pain, successful outcomes are rarely achieved by eliminating stiffness entirely. Instead, recovery depends on modulating protection, improving tissue tolerance, and progressively reintroducing load. TECAR, when integrated thoughtfully with neuromuscular re-education and movement-based care, serves as a practical bridge from early protection to confident return to training.